Why Teams Win and Lone Experts Lose
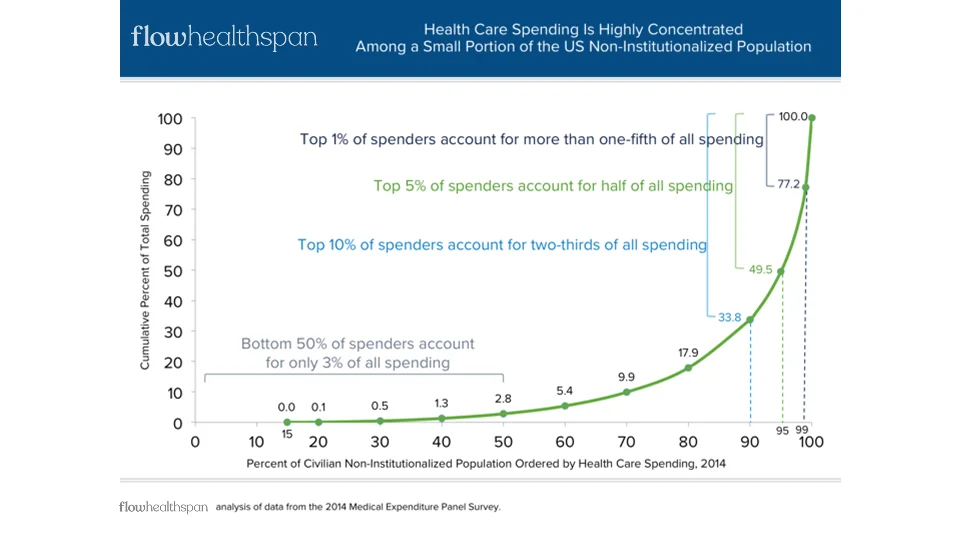
Longevity care asks a different question than traditional healthcare. It isn’t about resolving a single problem or delivering a discrete intervention—it’s about managing health, risk, and capability over time. That shift exposes a structural mismatch: systems built around individual experts and episodic services [/healthcare-finance-upside-down] are poorly suited to work that is continuous, cumulative, and cross-domain.
Even the most skilled professionals operate within narrow scopes. Financial advisors focus on capital and risk. Clinicians focus on diagnosis and treatment. Longevity practitioners focus on behavior, capacity, and daily execution. Each role is necessary, but none is sufficient on its own. When these disciplines operate independently, individuals are left to integrate decisions, reconcile tradeoffs, and manage conflicts between recommendations—effectively acting as the system without the tools, authority, or support to do so well.
Person-centered teams outperform lone experts not because individuals lack competence, but because longevity outcomes are produced through longitudinal coordination. Decisions compound over time. Financial choices shape care options. Care decisions influence functional capacity. Daily practices determine whether plans succeed or fail. Without a shared structure to align these domains, expertise fragments and outcomes degrade, and people are left with the burden of integration.
The Limits of Individual Expertise
Individual expertise excels at solving bounded problems. It breaks down when responsibility spans time, disciplines, and tradeoffs. In longevity care, no single professional can see—or own—the full picture. Attempting to centralize that responsibility in one professional role creates bottlenecks, blind spots, and unrealistic expectations.
This is why relying on a single professional, even exceptional professionals, doesn’t scale and doesn’t sustain. The issue isn’t effort or intent; it’s cross-discipline structural disintegration. When coordination is implicit rather than designed, it falls to the individual receiving care—adding burden precisely where clarity and support are most needed.
Longevity Care Is a Cross-Domain Function
Longevity care functions across domains simultaneously: financial planning, healthcare coordination, and ongoing longevity practice. These domains interact continuously, not sequentially. Treating them as separate services produces misalignment; treating them as a single function enables coherence.
A guided functional approach doesn’t replace expertise—it organizes it. Teams work from a single shared plan, common goals, and aligned incentives, while the individual remains the authority and active decider in their own care. The system exists to guide, coordinate, and adapt over time, not to substitute judgment or centralize control.
This is the foundation FLOW is built on—and why guides, roles, and incentives must be designed as a system rather than left disintegrated.
From Providers to Guides: How FLOW Roles Actually Work
Traditional healthcare systems are built around providers: licensed professionals delivering discrete services within defined scopes. That model works reasonably well for episodic care, but it breaks down when the objective shifts from treating problems to guiding long-term longevity, health, risk, and capacity. Integrated care requires continuity, coordination, and accountability across time—functions that sit outside the provider-only model.
FLOW distinguishes between providers, who deliver services, and guides, who help individuals plan, coordinate, and adapt those services over time. This distinction is foundational. Providers contribute expertise at specific moments. Guides support the individual as the constant, ensuring decisions remain coherent, sequenced, and aligned with long-term goals. Authority remains with the individual; guides exist to inform, structure, coordinate, and enable—not to replace judgment.
Guides
Guides are responsible for continuity. They work with the individual and other guides over time, helping translate goals into plans, plans into coordinated actions, and outcomes back into updated guidance. Their role is not to deliver every service, but to maintain alignment across domains as conditions, priorities, and constraints change.
In FLOW, guides are accountable to process quality and long-term outcomes rather than utilization or volume- that is the foundation of their relationship with the individual. They operate from a single shared plan, collaborate across disciplines, and help the individual navigate tradeoffs between financial, clinical, and longevity considerations without centralizing authority away from the person receiving care.
Providers
Providers deliver discrete, scoped services: clinical care, diagnostics, therapy, coaching, or instruction. Their responsibility is depth, not breadth. They engage when their expertise is required and disengage when it is not.
FLOW does not replace providers or redefine their scope. Instead, it integrates them into a broader system where their work is sequenced, contextualized, and supported. Providers remain autonomous within their domains, while benefiting from clearer context, better-prepared individuals, and reduced coordination burden—allowing professionals, particularly clinicians, to focus on practicing their craft and helping people, rather than managing friction imposed by the system around them.
Hybrid Guide–Providers
Some roles naturally span both guidance and service delivery. Financial advisors, primary care physicians in longitudinal models, and certain longevity clinicians may act as both guide and provider depending on context.
FLOW accommodates these hybrid roles without forcing artificial boundaries. What matters is not the title, but the function being performed at a given moment—whether the role is delivering a service or supporting planning, coordination, and adaptation over time.
Administrative Users- The Role Behind the Scenes
Administrative users support the system rather than the individual directly. This includes platform operations, compliance, billing, data management, and other necessary functions that enable coordination at scale- these roles are not guides or providers, but exist to enable them to do the meaningful integrated planning and service delivery required. In FLOW, administrative roles are deliberately separated from guidance and authority. Their purpose is to reduce friction, not introduce it—ensuring that professionals can focus on their work and individuals retain clarity, control, and continuity.
Guide Domains in FLOW’s Integrated Longevity and Healthcare Model
Longevity care spans multiple domains that operate continuously and interact with one another regularly over time. In FLOW, guidance is organized across three primary domains—not as silos, but as coordinated functions working from a single shared plan. Each domain has a distinct role, a different cadence, and a different form of leverage. Ordering matters.
Financial Guidance as the Primary Organizing Layer
Financial guidance provides the structural foundation for integrated care. It governs tradeoffs, sequencing, and feasibility—determining what is possible financially, when, and at what level of risk. Without this layer, even well-intentioned care plans become unstable, reactive, or misaligned with long-term goals and financial realities.
In FLOW, financial guidance is not downstream of care decisions. It is integrated into planning from the outset, shaping how healthcare and longevity investments are prioritized and sustained over time. This includes managing spending accounts, risk pooling, insurance integration, and long-horizon tradeoffs—always with the individual retaining authority over decisions.
By anchoring plans in financial reality, this domain enables the rest of the system to operate coherently and strategically rather than competitively.
Longevity Care Guidance
Longevity outcomes are produced primarily outside the clinic, hospital or doctor’s office. Daily behavior, physical capacity, nutrition, recovery, and resilience determine whether plans succeed or fail. Longevity and performance guidance translates long-term intent into sustained action.
This domain includes professionals such as personal trainers, nutrition coaches, medical doctors (for routine care), mobility and movement instructors, recovery specialists, and others who support physical and functional capacity over time. Their role is continuous and preventative rather than episodic, adaptive rather than prescriptive.
In FLOW, longevity guidance is not treated as ancillary or optional. It is a core function that closes the gap between planning and execution—feeding real-world feedback back into the system and allowing plans to evolve based on what is actually sustainable for the individual.
Using an old adage, an ounce of longevity care prevention is worth a pound of healthcare cure. This is why longevity care guides are secondary only to financial guidance.
Coordinated Healthcare Guidance
Healthcare guidance focuses on diagnosis, treatment, prevention, and clinical risk management. This includes physicians, mental health professionals, physical therapists in clinical roles, and other licensed providers whose expertise is essential at specific moments.
What changes in FLOW is not the practice of medicine, but its context. Healthcare guidance is coordinated with financial and longevity domains so that clinical decisions are sequenced appropriately, informed by long-term goals, and supported by surrounding capabilities. Mental health is treated as load-bearing rather than peripheral, and physical therapy spans both clinical recovery and functional longevity where appropriate.
By integrating healthcare into a broader guidance system, clinical expertise is preserved—and its impact extended.
How Guides Are Incentivized to Do Their Best Work
If longevity care requires coordination over time, then incentives must support continuity rather than throughput. Traditional fee-for-service models reward activity—visits, procedures, and utilization—regardless of whether those actions improve long-term outcomes. That structure distorts behavior, fragments care, and pushes coordination costs onto both professionals and individuals.
FLOW is designed around a different economic logic: guidance is valued as work in its own right. Guides are directly compensated for planning, coordination, longitudinal engagement, and outcome stewardship—functions that are essential to longevity care but largely unsupported in conventional systems.
Moving Beyond Fee-for-Service
In FLOW, compensation is decoupled from volume. Guides are not paid more for doing more things; they are paid, by the individual, to help them do the right things, at the right time, and for the right reasons. This enables professionals to focus on decision quality rather than throughput and to invest time where it has the greatest long-term impact.
By separating guidance from traditional service billing, FLOW reduces perverse incentives to overuse care while still integrating providers when their expertise is needed. The result is a system that supports restraint, sequencing, and prevention—without penalizing professionals for practicing responsibly.
Reducing Administrative Drag and Burnout
A significant portion of professional burnout stems not from the work itself, but from the systems surrounding it: billing complexity, documentation requirements, misaligned incentives, and constant friction between care and payment. These burdens erode time, focus, and meaning.
FLOW is designed to absorb much of that friction at the system level. By simplifying reimbursement pathways, clarifying roles, and aligning incentives across domains, guides and providers can operate closer to the work they were trained to do. The goal is not just efficiency, but sustainability—creating an environment where professionals can practice with autonomy, integrity, and a clear line of sight to the outcomes they are helping to produce.
What Coordinated Guidance Enables in Longevity Care
When guidance, incentives, and authority are aligned, integrated healthcare and longevity care stops relying on intensity or exceptional effort to succeed. Instead, outcomes emerge from structure: clear roles, prioritized financial capability, a single shared plan, and continuity over time. This shift benefits both the individual at the center of care and the professionals supporting them.
Better Outcomes Without Provider Heroics
In FLOW’s integrated and coordinated system, improvement does not depend on individuals navigating complexity alone or professionals compensating for systemic gaps. Decisions are sequenced, tradeoffs are explicit, and progress is measured across time rather than visits. This reduces unnecessary utilization while improving the likelihood that care and longevity investments compound as intended.
The result is not more intervention, but better timing, clearer priorities, and fewer failure points—allowing outcomes to improve through design rather than effort or expense.
Sustainable Careers and Scalable Care
For professionals, this model supports work that is both sustainable and meaningful. By valuing guidance, coordination, and long-term stewardship, FLOW creates space for deep expertise to be applied where it matters most—without constant administrative friction or misaligned incentives.
Because the system is designed around teams rather than individuals, it scales without depending on rare talent or burnout-driven intensity. Care improves not because people work harder, but because the system works better—for those receiving guidance and for those providing it.